What is PGT-A?
PGT-A (preimplantation genetic testing for aneuploidies) (Embryo testing) is a genetic test performed on embryos produced through ICSI. PGT-A gives information about embryos’ genetic health to help your care team select the best embryo for transfer and improve your chance of achieving a successful pregnancy. PGT-A was formerly known as PGS, preimplantation genetic screening.
All data is collected from Igenomix. These studies were not conducted at Generation Next Fertility. Please see more information here: https://www.igenomix.com/our-services/pgt-a/
Normal Chromosome Number
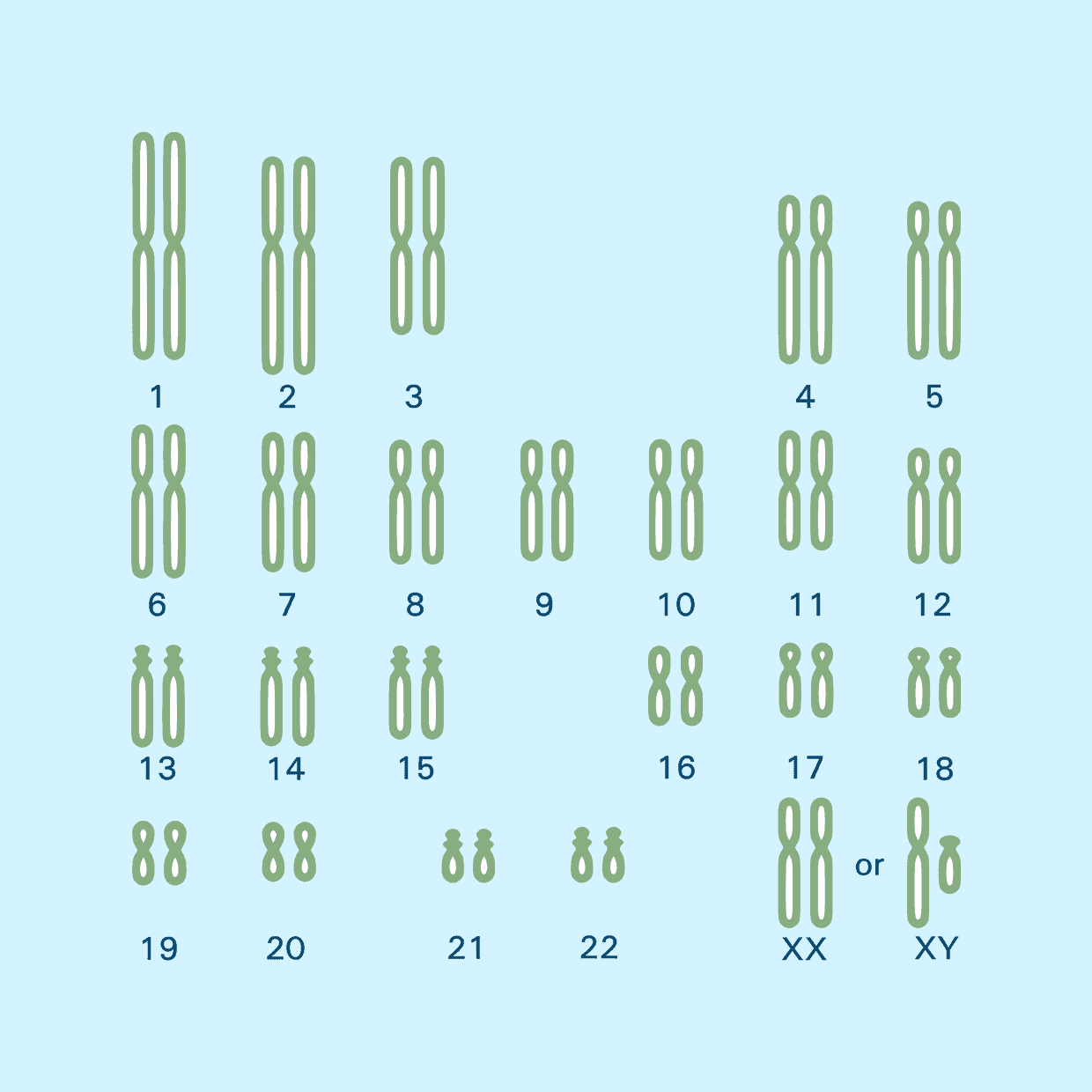
Abnormal Chromosome Number

Do my chances of having an aneuploid embryo increase with age?
Yes, The chance of having an abnormal embryo increases with maternal age. The chance of aneuploidy for each blastocyst embryo based on maternal age is as follows:
- 43% for women between the ages of 25-30
- 45% for women between the ages of 31-34
- 54% for women between the ages of 35-37
- 65% for women between the ages of 38-40
- 71% for women between the ages of 41-42
- 80-90% for women between the ages of 43-46.
All data is collected from Igenomix. These studies were not conducted at Generation Next Fertility. Please see more information here: https://www.igenomix.com/our-services/pgt-a/
What do my results mean?
Embryos will be identified as chromosomally normal (46 chromosomes) or abnormal. PGT-A also screens for aneuploidies involving the sex chromosomes. If the patient does not want the sex of the embryos to be reported, they must notify the staff in advance.
Normal:
Embryos diagnosed as normal are good candidates for transfer as they are most likely to result in a successful pregnancy.
Abnormal:
Embryos diagnosed as aneuploid are not recommended for transfer. There is the possibility that all embryos analyzed will be chromosomally abnormal. This possibility is more likely when there are fewer embryos to analyze and with older women whose aneuploidy rates are higher.
Inconclusive:
There is a possibility of inconclusive results for an individual embryo due to lack of DNA or poor DNA quality.
Re-biopsy and re-testing of embryos with inconclusive results may be discussed with the physician.
The PGT-A Process
Are There Risks?
Data shows that embryo biopsy is not associated with an increase in fetal abnormalities or birth defects compared to IVF without embryo biopsy.
There has been no documented decrease in implantation rates with embryo biopsy. The chance of hurting the embryo is about 1% during the biopsy stage due to the requirement of assisted hatching for PGT.
The majority of embryos survive the biopsy but studies investigating the long-term consequences of embryo biopsy are limited.
There is a general risk of birth defects of 4-6% for any baby born following IVF treatment. Birth defects may be caused by genetic or non-genetic etiologies.
Are there alternative options?
Non-invasive prenatal testing is an alternative prenatal option, but may also have false negatives and false positives. Prenatal testing options can be discussed with the obstetrician PGT-A cannot detect birth defects directly.
There is a general risk of birth defects of 4-6% for any baby born following IVF treatment. Birth defects may be caused by genetic or non-genetic etiologies. PGT-A cannot detect single gene disorders such as cystic fibrosis, sickle cell anemia, or Tay-Sachs disease. Carrier screening can help identify couples who are carriers for a single gene disorder, even when there is no family history of that condition.
The PGT-A Process
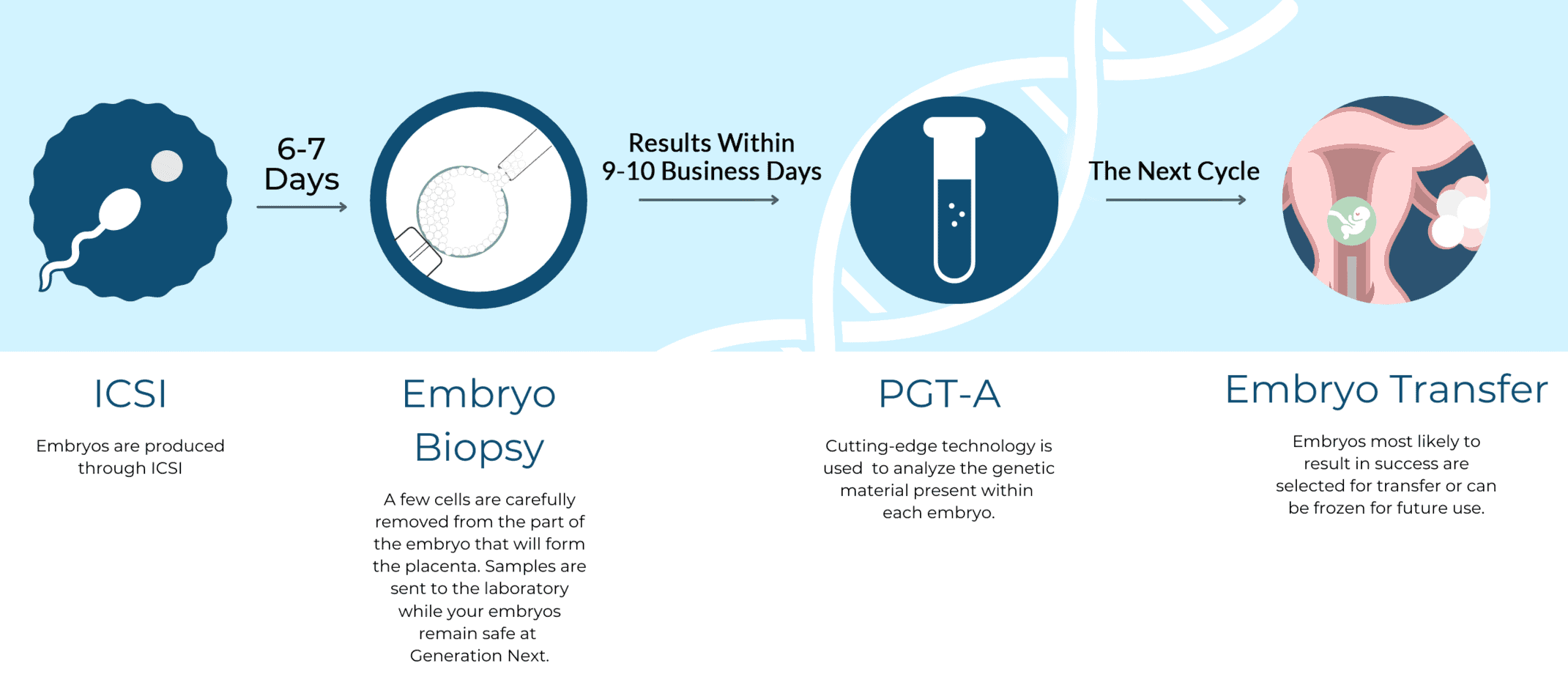
Are PGT-A Tests Accurate?
Results of PGT-A testing are 98% accurate. There remains a 2% chance of a misdiagnosis, either by a false negative or a false positive result.
When can a misdiagnosis occur?
Misdiagnosis can occur when the cells biopsied and tested do not represent the embryo as a whole (mosaicism). Because of this possibility, prenatal diagnosis (CVS or amniocentesis) is always recommended to confirm the results of PGT-A.
Can PGT-A detect single gene disorders?
PGT-A cannot detect single gene disorders such as cystic fibrosis, sickle cell anemia, or Tay-Sachs disease. Carrier screening can help identify couples who are carriers for a single gene disorder, even when there is no family history of that condition.

Are There Risks?
Data shows that embryo biopsy is not associated with an increase in fetal abnormalities or birth defects compared to IVF without embryo biopsy.
There has been no documented decrease in implantation rates with embryo biopsy. The chance of hurting the embryo is about 1% during the biopsy stage due to the requirement of assisted hatching for PGS.
The majority of embryos survive the biopsy but studies investigating the long-term consequences of embryo biopsy are limited.
There is a general risk of birth defects of 4-6% for any baby born following IVF treatment. Birth defects may be caused by genetic or non-genetic etiologies.
Are there alternative options?
Non-invasive prenatal testing is an alternative prenatal option, but may also have false negatives and false positives. Prenatal testing options can be discussed with the obstetrician PGT-A cannot detect birth defects directly.
There is a general risk of birth defects of 4-6% for any baby born following IVF treatment. Birth defects may be caused by genetic or non-genetic etiologies. PGT-A cannot detect single gene disorders such as cystic fibrosis, sickle cell anemia, or Tay-Sachs disease. Carrier screening can help identify couples who are carriers for a single gene disorder, even when there is no family history of that condition.


