Platelet Rich Plasma (PRP)
What is PRP?
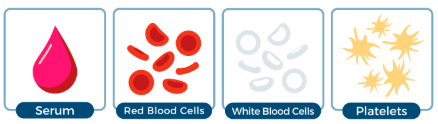
There are 4 main components in your blood:
Serum, Red Blood Cells, White Blood Cells, and Platelets.
When an injury occurs, platelets release growth factors that stimulate regeneration, repair damaged tissues, and reduce inflammation. These processes are essential for maintaining the body’s ability to heal itself.
Platelet-Rich Plasma (PRP) Therapy builds on this natural mechanism. By isolating and concentrating platelets from your own blood, PRP creates a treatment that may promote tissue repair and regeneration.
PRP has been widely used in medical specialties such as orthopedics, dermatology, and sports medicine for decades. It has been used to treat joint injuries, accelerate post-surgical recovery, and even rejuvenate skin in cosmetic procedures like the “vampire facial.” Now, its potential in reproductive medicine is being explored, offering new possibilities for addressing fertility challenges.
How is PRP Made?
PRP is created using a simple and minimally invasive process. A small amount of blood is drawn, much like during a routine medical visit. This sample is then placed into a centrifuge, which spins the blood at high speed to separate its components. The resulting plasma, rich in platelets, is carefully extracted and prepared for use.
Once prepared, the PRP is injected into targeted areas, such as the ovaries or uterine lining, where it may stimulate tissue repair and regeneration. Because PRP is derived from your own blood, there is no risk of allergic reaction or rejection, making it a biocompatible and natural option.
In fertility care, PRP is being studied as a potential way to support ovarian tissue and enhance the uterine lining, offering hope for individuals with diminished ovarian reserve (DOR) or thin endometrial lining.
PRP as a Fertility Treatment
PRP therapy is an experimental treatment aimed at addressing specific fertility challenges. It is currently being studied for its potential to improve ovarian function in individuals with diminished ovarian reserve, enhance the uterine lining’s thickness and receptivity, and increase the likelihood of developing chromosomally normal embryos.
Generation Next Fertility offers two applications of PRP in fertility care: Endometrial PRP and Ovarian PRP.

Endometrial PRP
Endometrial PRP is designed to improve the thickness and health of the uterine lining, which is essential for successful embryo implantation. During this procedure, PRP is infused into the uterine cavity using a catheter.
This treatment is generally considered for individuals with a thin uterine lining (often defined as less than 7 mm), recurrent implantation failure, or those preparing for an embryo transfer. In some cases, multiple infusions may be performed within a treatment cycle to encourage better lining development.
Ovarian PRP
Ovarian PRP involves injecting PRP directly into the ovaries under ultrasound guidance. The growth factors in the PRP may stimulate dormant follicles and improve the ovarian environment, potentially leading to better egg quality and quantity.
Ovarian PRP is often explored by patients with diminished ovarian reserve (DOR), poor ovarian response (POR), or advanced maternal age with associated declines in egg quality. The procedure is typically performed one to three months before starting an IVF cycle to allow time for the ovaries to respond.
Ovarian PRP: The Future of Fertility
PRP is created using a simple and minimally invasive process. A small amount of blood is drawn, much like during a routine medical visit. This sample is then placed into a centrifuge, which spins the blood at high speed to separate its components. The resulting plasma, rich in platelets, is carefully extracted and prepared for use.
Once prepared, the PRP is injected into targeted areas, such as the ovaries or uterine lining, where it may stimulate tissue repair and regeneration. Because PRP is derived from your own blood, there is no risk of allergic reaction or rejection, making it a biocompatible and natural option.
In fertility care, PRP is being studied as a potential way to support ovarian tissue and enhance the uterine lining, offering hope for individuals with diminished ovarian reserve (DOR) or thin endometrial lining.
DR. JESSE HADE
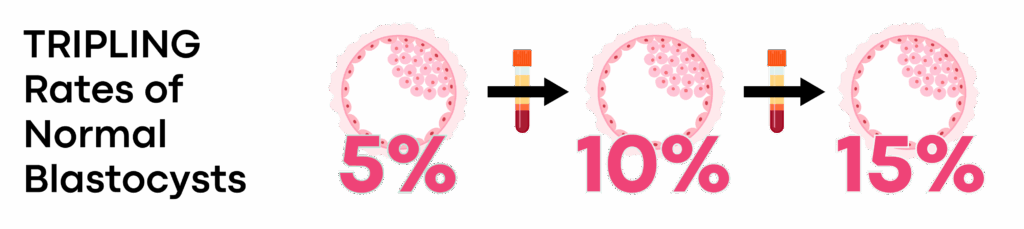
In our preliminary data, we’ve examined 22 patients who have gone through IVF And PRP. What we’ve identified in these individuals that – which was amazing and really is what’s driving our study – is that we found that the chromosomal normalcy rate in blastocyst went from 5% in the First Cycle (Prior to starting PRP) going to 10% and then eventually 15% with each subsequent additional PRP Therapy.
Once prepared, the PRP is injected into targeted areas, such as the ovaries or uterine lining, where it may stimulate tissue repair and regeneration. Because PRP is derived from your own blood, there is no risk of allergic reaction or rejection, making it a biocompatible and natural option.
In fertility care, PRP is being studied as a potential way to support ovarian tissue and enhance the uterine lining, offering hope for individuals with diminished ovarian reserve (DOR) or thin endometrial lining.
Fertility Rejuvenation
From hormones and egg counts to dosage and timing, fertility care begins by understanding what makes each body unique. At Generation Next Fertility, that individuality guides how our providers tailor care: by selecting the approaches most likely to work for each patient rather than relying on standardized protocols alone.
For some patients, such as those with lower egg reserves or a history of failed transfers, improving success rates may require looking beyond medications alone and toward how the reproductive environment itself can be supported.
That’s why researchers have been exploring regenerative approaches, like Platelet-Rich Plasma (PRP),
that may help enhance ovarian and uterine conditions in select cases.
Long used in fields such as orthopedics, dermatology, and sports medicine to support tissue repair, PRP involves concentrating a person’s own platelets and delivering them to targeted areas.
That’s why researchers have been exploring regenerative approaches, like Platelet-Rich Plasma (PRP),
that may help enhance ovarian and uterine conditions in select cases.

Innovation Made Accessible
At Generation Next Fertility, PRP is offered as part of our commitment to staying at the forefront of reproductive research. By giving patients access to emerging scientific approaches, we not only expand today’s treatment possibilities, but also contribute to the work that may one day make therapies like PRP a standard, insurance-covered part of fertility care.
The Steps

1. Schedule a consultation
In-Person & Telehealth available.
Click here to get started!

2. Send us your insurance info
While PRP is not covered by insurance, other parts of your care may be.

3. Meet with our team
Find out whether PRP may benefit your specific case.

4. Know what’s ahead
Understand how PRP fits within your treatment plan’s next steps.
How PRP Supports Fertility
PRP is used in fertility care in two distinct ways, depending on which part of the reproductive system may benefit from additional support. Consideration is based on a patient’s specific clinical profile and treatment goals.

Endometrial PRP is placed in the uterine lining, with the goal to create a more receptive environment for implantation.

Ovarian PRP is placed into the ovary tissue, with the goal of supporting egg, follicle, and embryo development.
PRP explained
in 60 seconds
“Can PRP help with
low ovarian reserve?”
“I haven’t started IVF yet,
can I do PRP right away?”

Research & Discounted IVF
Generation Next Fertility is conducting the leading clinical studies evaluating how Ovarian PRP may be applied to support ovarian health and embryo development. Pricing below reflects the self-pay rate; select services may be eligible for insurance coverage.
2 IVF Cycles for $12,000
This clinical trial tests Ovarian PRP against placebo to study its effects on the ovaries and whether it improves IVF outcomes.
You may be eligible if you have DOR, POI, or Failed IVF history. Participants may or may not receive PRP.
Get 2 IVF Cycles for $17,500
This clinical trial uses CHLOE™ AI imaging technology to assess how Ovarian PRP may influence embryo development and quality.
You may be eligible if you have not been diagnosed with DOR. All participants receive PRP.